A faster horse
Fixing the EHR, Part 5
I’ve been doing Medicine for over forty years now. But 15 years before I graduated, Lawrence Weed MD published an article in the New England Journal of Medicine that hugely changed how we view and do Medicine. It was called Medical Records that Guide and Teach.1
He almost got it right. Here’s how his article begins:
The beginning clinical clerk, the house officer and the practicing physician are all confronted with conditions that are frustrating in every phase of medical action. The purpose of this article is to identify and discuss these conditions and point out solutions. To deal effectively with these frustrations it will be necessary to develop a more organized approach to the medical record, a more rational acceptance and use of paramedical personnel and a more positive attitude about the computer in medicine.
The good bits
The ‘good bits’ of Weed’s enterprise are very good. He anticipates how beneficial computers may be if we wish to do medicine well. He is nothing if not thorough. He firmly and correctly advises us to build our record around the actual problems the patient has. He gives us the “problem-oriented record”, a brilliant idea. He says how important it is to appreciate the patient’s demography. He emphasises continuity of care, proper organisation of data and audit of doctors’ work.
But the approach many people grabbed eagerly is called ‘SOAP’. It was revolutionary at the time, but is now commonplace. First write down what the patient said (‘subjective’ information), then what the clinician found (‘objective’ data, together with lab tests and so on), next the clinician’s assessment, and then their plan. S.O.A.P.
This is now the way that many junior doctors are taught to “do medicine”, and it sticks. It’s systematic. It stores important information and thinking. But there’s a problem.
A stumble
In some areas of human endeavour, “almost right” is indistinguishable from “catastrophically wrong”. A big problem with SOAP is that it seems to encourage linear thinking.2
S ⟶ O ⟶ A ⟶ P. Done.
In fact, Weed goes one step further out of line. Here he is:
In the face of the confusion concerning the necessary quantity of data, the initial collection of data should be made as significant and complete as possible. The only limitations should be the discomfort, danger and expense to the patient.
What’s wrong with this? Let’s make a brief digression. It concerns …
What is Good Medicine?
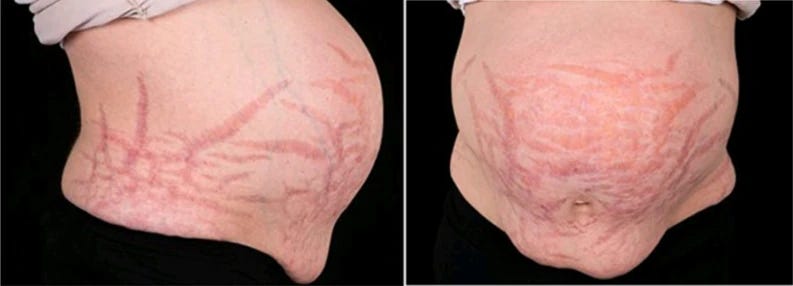
Experienced doctors get very good at spotting patterns. Take the picture above. While the student is still putting together the patient’s unfortunate tendency to get recurrent infections, their prematurely thinning bones, and their early diabetes, the experienced physician has already noticed their ‘buffalo hump’, examined their tummy for the 2 cm-wide striae she knew would be there, and said “Cushing’s”.3
At this point, don’t get me wrong! This experienced doctor may be doing Good Medicine, or they may simply be falling into another trap. The experienced clinician will rapidly make a diagnosis, often with remarkable ease. The Good clinician will then immediately question their own diagnosis.
They will try to disprove the diagnosis of “Cushing’s syndrome”. Here’s where it becomes technical. For example, they will do a baseline early-morning blood cortisol level, give the patient one milligram of dexamethasone at midnight, and then repeat the blood test the next morning. If the cortisol level is now suppressed from an initial high, they have disproved their hypothesis. Otherwise, further tests are warranted.
We know how this works, because we understand Good Science.⌘ And Good Science and Good Medicine are—or should be—best friends.
Science starts with problems, which we try to explain. We then brutally cut down the explanations (theories) that don’t work by trying hard to refute them. We’re left with provisional but well-tested theories we can act on. We then re-evaluate the results of our actions, and repeat the cycle. New problems arise.
Weed’s stumble
I’m afraid that Weed doesn’t do Good Science. His approach is “data driven”! In fact, he’s rather rude about a scientific approach of selectively ordering indicated tests. Instead, he wants to grab more labs early on, and whack them into a computer. According to him, hypothesis generation can only follow on comprehensive acquisition of lots of data.4 I’ve previously explored the muteness of data.⌘
Science starts with problems, not ‘data’. We then try to disprove our cherished hypotheses. Think the patient with the problem of chest pain might have a new myocardial infarction? If the serum high-sensitivity troponin is not raised, you’re wrong. Think the patient with the problems of breathlessness and a fast heart rate might have a pulmonary embolism? If an appropriately taken D dimer is negative, then you’re wrong. Posit that the patient with leg swelling and lung crackles has heart failure? If the n-terminal proBNP level is 20 pmol/L, you’re almost certainly wrong.5
Science isn’t a horse race, with a start and a finish. Science is not linear. No theory (or diagnosis) is cast in stone. Re-evaluation is continually needed. The process is cyclical.6
Computerisation
I’ve dwelt on Weed’s failings, because they are common and important. If you don’t get your basic plan right, computerising your wrong approach will simply crystallise your dysfunction in silicon. This has happened in the past. This is what continues to happen, pretty much wherever someone says “Computerise Medicine? Should be easy. Let’s begin!”
We have the advantage of knowing how to do it right. Let’s Science it.⌘ First, to summarise a recent post,⌘ I started by emphasising the importance of PEOPLE and attaching and safeguarding their PERSONAL attributes. We’ve also identified how to record PROCESSES over time, describe individual interactions between caregivers and people, and build expressive structures by relating processes to one another (meta-processes).
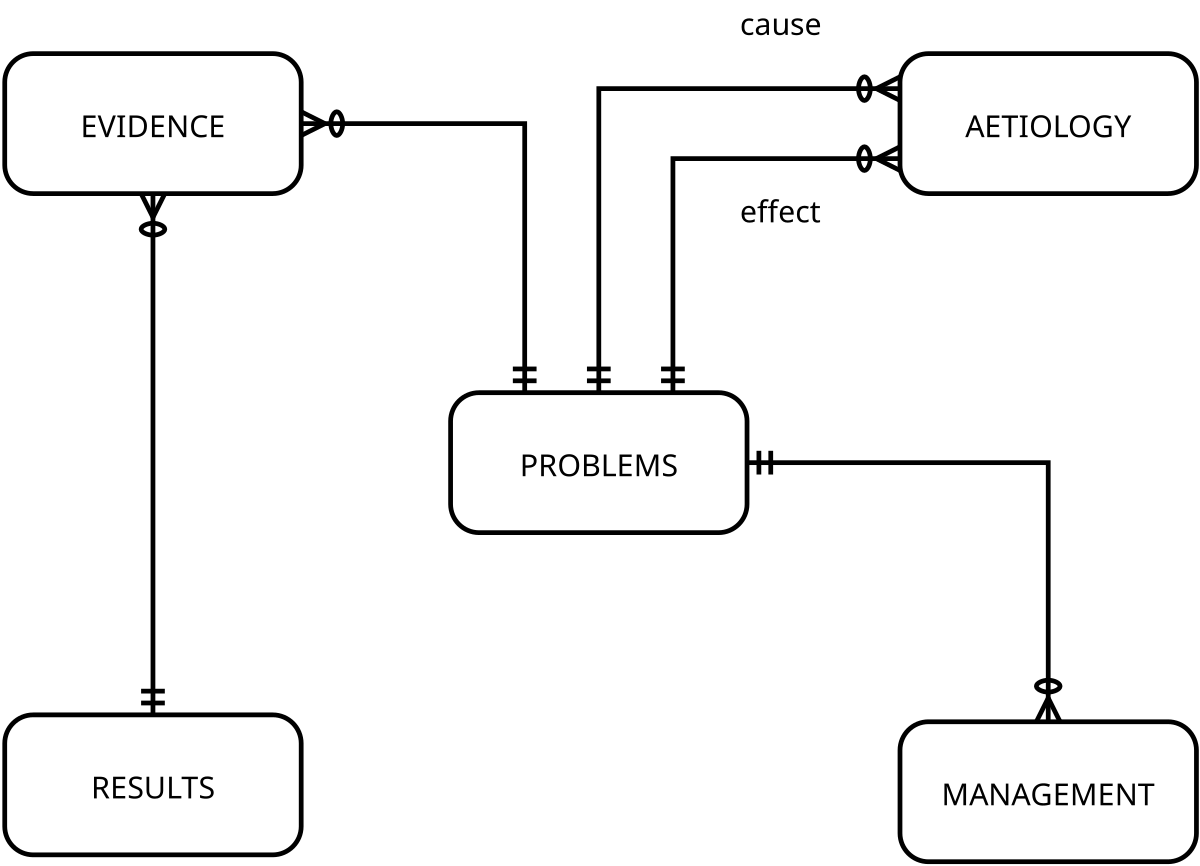
We’ll now put together many of the remaining building blocks that are needed to turn this sketch into Science. Starting with problems. Consider the diagram above. The rather peculiar “crows’ feet” reflect relationships between the ‘entities’ in boxes.7
PROBLEMS are indeed central. Weed’s problem-oriented record. Naturally, problems can cause other problems, for example Cushing’s syndrome can cause high blood pressure, and high blood pressure can cause heart failure, and heart failure can cause shortness of breath. To accommodate this long chain of causality, we create an AETIOLOGY table that relates a cause to an effect. A simple solution, but also a way to code causal hypotheses.
Problems demand evidence that they exist, and indeed evidence that they have not been refuted. So our EVIDENCE table links RESULTS to PROBLEMS, saying why we decided what we did.8
Problems also engender solutions. So we need some sort of MANAGEMENT table that describes how we’ve responded to individual problems. This is a decent start, isn’t it? Let’s fill in more gaps …
Closing the circle
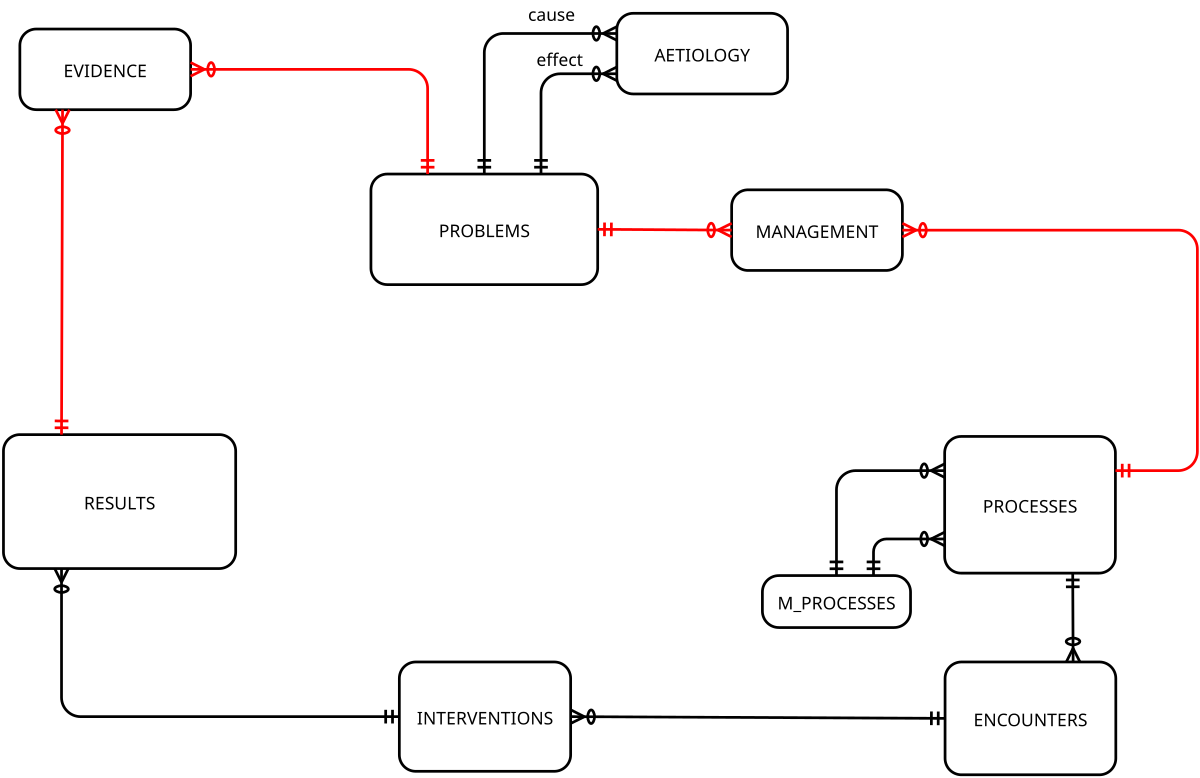
The above diagram links in our existing PROCESSES, ENCOUNTERS (a one-to-one interaction between a caregiver and a patient)9 and meta-processes, with an extra table that’s rather important: INTERVENTIONS.
The important feature of the above linkage is that it goes around and around! Like Science. Just like Science. Problems are linked to processes by the MANAGEMENT table; each ENCOUNTER will result in the carer doing something—an intervention. This will necessarily produce RESULTS, whether these are observations, measurements, investigations, or simply a record of something that was done, for example the dose of a drug that was administered.
These RESULTS then inform assessment of PROBLEMS through the EVIDENCE table, and we’re back to ‘Doh’. Science goes round and round.
A faster horse
There is no evidence that Henry Ford ever said the fabulous words:
“If I had asked people what they wanted, they would have said faster horses”.
But today we are being offered faster, data driven horses, whether we like it or not. The dreadnought of badly-done medicine⌘ is given a data-driven push. The patient becomes a Victim Of Modern Investigative Technology in the Palace of Iatrogenesis.⌘
If the underlying design of our swanky modern electronic health records is based on bad science, they will tend to stumble and let us down when we most need them. Computerising the wrong approach just makes the falls faster and more dangerous. We do require medical records that guide and teach, but we must design right. It’s not a race. It’s not linear. Good Science involves a cycle of progressive re-examination.
I’ve argued that part of the ‘basics’ is building the information layer so well that it almost never needs to be re-designed. The functional layer can then be loosely coupled to it,⌘ allowing ongoing improvement. We’re now well on the way to doing this.
We still have a fair bit of work to do in the next several posts. One thing you might have noticed is that I omitted the PEOPLE table from the above diagram. This is mainly because it already links to all of the tables, often in several different ways. We will initially keep our diagrams very simple.
Other observant readers will recall that in my most recent post in this series⌘ I initially promised a description of how we can incorporate the multiple dimensions of SNOMED⌘ into our record design. I have not yet fulfilled this promise. This is because after speaking to several people smarter than myself, I realised that it’s better to properly articulate most of the skeleton first. Science encourages critical review. I’ve just done so. In my next post, I’ll keep the promise I made earlier.
My 2c, Dr Jo.
⌘ This symbol is used to indicate posts where I’ve discussed the flagged topic in more detail.
The image at the start was poorly constructed by Ideogram (giving the horse five legs and a half-robot rider) and then partially fixed using Gemini’s Nano banana. It also introduced the stumble on request.
Naah. the NEJM churlishly wants to charge you to read it. But if you look around, you can find copies on the Web.
There are are actually several problems with Weed’s approach. His choice of distinguishing categorically between ‘Subjective’ and ‘Objective’ is traditionally Cartesian, and ignores the fact that an objective position is impossible. As you might expect, he also ignored the potential for the patient participating in the record, which would have been heretical at the time.
The link is the source of the picture.
Weed’s approach is also mathematically naive. Simple maths tells you that if you have 60 facts, there are 60! ways you can combine them. That’s more ways than there are atoms in the known universe. This is computationally intractable.
Of course I’m preaching here. And of course if you take a Bayesian approach, a BNP of 600 massively changes the posterior odds of this being heart failure. The important point is that we embed self-critical thinking in the mechanism of Science. That’s why I’m preaching.
Interestingly enough, the military OODA approach (observe, orientate, decide, act) is formulated to speed cognitive adaptation in changing circumstances. It’s designed to work in circles of re-evaluation; you can see the similarity to both my ‘Good Science’ and the ‘Shewhart (PDSA) cycle’.
The symbols indicate a minimum and maximum number, for example —○|— translates to “A minimum of none, and a maximum of one”; the actual ‘crow’s foot’ i.e. ⋔ means “many”. I’ve been naughty in the diagram: technically the ‘entities’ should be square boxes with lists of properties. This will come much later.
We might even weight the strength of our certainty using a Bayesian approach.⌘
The terminology is fraught. We may end up spending a whole post on ‘epochs of care’ versus ‘encounters’ and ‘episodes of care’; we may likewise agonise for days about ‘problems’, ‘conditions’, and so on.


"Computerising the wrong approach just makes the falls faster" This applies to nearly every project I have worked on, none of them in medicine! If you tell the customer that first they need to do some serious business process analysis they look at you as if you have two heads. Then spend a fortune with SAP because the salesman said SAP can do anything.
If you would only convert medical records to SAP iDocs I am sure it would just work out fine :-)
Eagerly waiting the incorporation of PEOPLE, because I am different than others (intelligence, belief, experience), and I am part of the equation.